2011 April blog
Reggie Annan

This month I write about food taboos in Africa, and their impact on diets and health. Then I interview Elias Kumbakumba, a paediatrician at the Mbarara Referral Hospital, Uganda, on how to tackle malnutrition. My mood picture this month is of sunrise on the Nile, generally accepted to be the longest river on Earth, at 6,695 kilometers (4,160 miles), from Lake Victoria, 1,140 metres above sea level at Jinja, the second largest city of Uganda, to its delta in Egypt. Read more at http://www.shunya.net/Pictures/Uganda/Jinja/Jinja.htm.
Food and culture
African food taboos

Anything that is taboo (a Polynesian word) is strictly forbidden, for cultural or spiritual reasons. Those known to have transgressed taboo are punished, and may be cast out of their society. The Christian Old Testament includes many ordinances on forbidden foods. These days, taboo is usually seen as a magic concept with no real basis. But there often is reason for it, at least within systems of belief, some of which are now termed 'religions', others 'philosophies', and others 'superstitions'.
In Africa, as in many other parts of the world, what people say and do is strongly influenced by age-old supernatural beliefs, which Christian missionaries downgraded as 'superstition'. In Africa, as in Asia, older and country people still may live as much in the realms of the supernatural and the afterlife, as in the physically living realm. When I was young in Ghana, my friends and I were forbidden to go into dark forests such as that shown above. We were given spiritual reasons for this. The absolute prohibition also made good practical sense.
One of the classic food taboos I knew about whilst growing up in Ghana was that when children were fed eggs, they grew up to become thieves. Hence it was forbidden to give eggs to children. It was not unlikely for children to warn other children eating boiled eggs that they would become thieves. Yet some children would completely refuse even if they were offered eggs because they did not want to end up as thieves. Women also avoided certain foods when pregnant in certain cultures out of fear and belief that certain foods could harm unborn children.
These beliefs pertained in many other African tribes. In the Bugosa district of Uganda, females and female children over 6 years were forbidden to consume eggs, poultry, mutton, pork and certain kind of fish (1). In the Bukedi district, females were forbidden to eat eggs, chicken and pork. Similar restrictions were kept by the Bantu tribes, who also believed that children could become stupid by consuming yam, a root (1). Eggs, chicken, fish, pork and goat's milk were forbidden for females in the Ankole district (2). Below is a photo of various African dishes. Some of these may not be eaten because they are forbidden.

Food taboos are deeply entrenched. Their rationale may be religious, cultural, hygienic, historic or economic. For instance as I grew up, I asked how could it be that feeding children eggs made them thieves. The explanation was that it was for economic reasons, especially among the poor. In those days eggs were luxuries. People feared that when children were fed very well or were brought up luxuriously, they would resort to stealing to maintain opulent ways of living when their parents can longer afford or when they grew up. And so to avoid this situation, children were not allowed foods considered to be luxuries. The taboo made sense.
These taboos can also be due to historical reasons. For instance a royal family in Ghana refused to eat pigeon, because they believed an ancestor of theirs was once helped by a pigeon to win a battle. Among some nomadic livestock herders, refusal to eat fish was to scorn the ways of life, the culture, of fishing communities. Pork and alcohol were also forbidden for religious reasons.
Food taboos have an impact on dietary intake and nutritional status. In Uganda, tribal food taboos, especially as applied to women and female children, have been one of the main causes of malnutrition (4). In Togo, West Africa, poverty, ignorance together with food taboos were related to a lack in weaning food varieties (5), probably because most of the nutritious weaning foods were forbidden.
Taboos are a cause of kwashiorkor
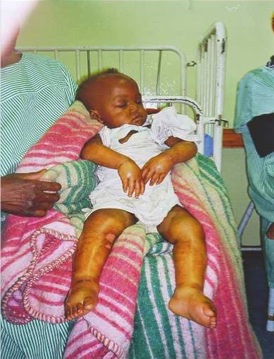
Kwashiorkor, a form of severe acute malnutrition, is the result partly of taboos around feeding children. Kwashiorkor is a 'Ga' word from the 'Ga' tribe in the South Coastal region of Ghana, where I come from. It is a name attached to second girl children in one of the clans in this tribe. More generally, it has been used by the local people to describe the disease of the first child as a result of the coming of the second child. In severe cases, such as shown in the picture above, children with kwashiorkor have in addition to oedema (swelling), apathy and irritability, some skin lesions and burns known as dermatosis and hair changes.
How did kwashiorkor come about?
Let me give you a little bit of the history of this condition. In Ghana, it was forbidden for a mother to continue breastfeeding her child when she became pregnant with another child, even if the child was only six months old. This is still the case to a large extent though the word 'forbidden' is too strong, 'frown upon' is more accurate now. Such mothers stopped breastfeeding as soon as they got pregnant. These children did not just stop breastfeeding, but were often neglected because mothers turned all their attention on the pregnancy and preparation for the coming child. Hence the first child became malnourished.
The indigenous people in those days apparently did not realise that these children were suffering from malnutrition because they had been prematurely weaned, were inadequately fed, and received poor care. It was Dr Cicily Williams, a paediatrician originally from Jamaica, who in the early 1930s worked in Accra, Ghana, and observed this phenomenon among the local communities. She later made this condition known to the medical world and kept the term 'kwashiorkor', already used by the indigenous people of the Coastal Accra region of Ghana to describe the condition.
In addition, I think embarrassment that a woman was breastfeeding and also pregnant, has been a factor. I am saying this because I myself come from the Ga tribe, and as a young person I knew that there was some stigma attached to breastfeeding whilst pregnant. Thankfully most women in Ghana, including those in the Ga tribe, through formal education, enlightenment and civilisation, now know that a child suffering from kwashiorkor is a malnourished child. Family planning and child spacing mean that fewer mothers become pregnant too soon after giving birth. Although some children still suffer from kwashiorkor, people are generally aware of its causes.
Food taboos persist
Earlier in recent history in Africa, many food taboos were respected and observed in Africa. It's hard to say how many of them survive now. In the 1960s it was thought that most of the taboos among tribes in Uganda were observed mainly among the uneducated, and were ignored by the educated. But sometimes educated people keep to their old customs quietly.
In 1998, Association member Joyce Kikafunda and colleagues assessed dietary and environmental factors influencing stunting and other signs of poor nutritional status of children <30 months of age in a central Ugandan community. They found that food taboos were not associated with stunting and other indicators of poor nutrition (5). Rather, the main causes of poor nutrition in rural communities included poor health, the use of unprotected water supplies, lack of charcoal as fuel, lack of milk consumption, lack of personal hygiene, general impoverishment, poor education of the mother, consumption of food of low energy density, and lack of meat and cow's milk consumption.
In Malawi however, it was recently reported that food taboos resulting from cultural and religious beliefs still limit the use and consumption of certain foods, hence reducing food diversity at the household level (6).
Food taboos are a relatively neglected issue. It is very important that they be identified, understood and addressed, especially in countries with high levels of food insecurity. It should never be assumed that taboos are just a product of stupidity and ignorance. Their rationale may be of a type that most people now think makes no sense, but all religions have a supernatural aspect. It may well be that a key to reducing food insecurity is addressing food taboos and expanding food choices. Levels of micronutrient deficiencies among children and women in Africa are still high. Food taboos that lead to monotonous diets could well be a cause. We need to know more about this absorbing, important and sensitive topic.
References
- Burgess HJL. Protein-calorie malnutrition in Uganda, II-Busoga District, III-Bukedi District, IV-Bugisu District, V-Ankole district. East African Medical Journal 1962:39
- Rutishauser IHE. Custom and child health in Buganda.Tropical Geographic Medicine 1962, 15: 138-147.
- Cleave JH. Food consumption in Uganda. East African Medical Journal 1968, I: 70
- Excler JL, Nicolas E, Mojon M. Protein-energy malnutrition in an urban African milieu (Togo). Etiologic factors in kwashiorkor and marasmus-kwashiorkor. ]ournal of Tropical Medicine 1985; 45(2):155-61.
- Kikafunda JK, Walker AF,Collett D, Tumwine JK, Risk factors for early childhood malnutrition in Uganda. Paediatrics 1998, 102 (4): e45.
- 6 KainjaJ Malawi Food Security. 2009. Accessed at http://jimmykainja.co.uk/malawi-food-security/
Ugandan children
Malnutrition: a paediatrician's view

In February I interviewed Florence Turyashemererwa, a nutritionist from Uganda who shared her experiences in working as a nutritionist in Uganda. Flo told us how her commitment to ensuring appropriate treatment of malnourished children admitted to the Mbarara Referral Hospital (pictured above) led to the establishment of a nutrition ward, procurement of adequate food, and implementation of the WHO guidelines for the treatment and prevention of malnutrition. These changes resulted fewer deaths from malnutrition and prevention of recurrence. The achievements gave renewed hope and empowerment to mothers and carers who hitherto felt hopeless and powerless.

This month I interview Elias Kumbakumba, pictured above. He talks from a clinician perspective on caring for children with malnutrition in Uganda, and the ways forward to address and eradicate malnutrition among Ugandan children.
Please tell us a bit about yourself
I am a paediatrician in Mbarara Regional Referral Hospital and a lecturer in Mbarara University of Science and Technology. This is a medical school that trains community oriented medical workers and doctors, where I also trained. I have six years' work experience, most of this with children mainly with acute tropical infections, often coexisting with malnutrition of different degrees. I am also involved in research in the faculty mainly in malaria and tuberculosis. I was involved in the establishment of a feeding programme four years ago that has now changed the lives of many children with severe malnutrition.
What is the malnutrition situation among children in Uganda in general and in the hospital you work at?
The national rate of stunted children stands at 38 per cent, and of underweight 16 per cent and wasting 6 per cent. The proportion of children with chronic malnutrition in Uganda is highest in South-Western Uganda with almost 50 per cent of under-5s being affected (1). Similarly this region falls behind others in other nutritional status indicators. A survey at the Mbarara Regional Referral Hospital (which is in south western Uganda) in 2007 showed that close to 60 per cent of all hospitalised children had evidence of malnutrition and 25 per cent had severe life threatening malnutrition. At our hospital, an estimated 13 per cent of all children admitted with severe acute malnutrition died in 2007, and 9.1 per cent in 2009 (These records are not published).
Facility-based rehabilitation for severe malnutrition requires one month on average, a duration, which many mothers cannot accommodate due to family, social, and economic constraints. Our nutrition centre treats about 200 children with severe malnutrition annually. This is just a tip of the iceberg.
HIV/AIDS has aggravated malnutrition
How would you grade the impact of HIV infection on malnutrition in these children?
While there are many children with pure malnutrition coming to our centre, HIV/AIDS has compounded the problem significantly. Hospital stay and mortality is much higher in these children. Between 40-50 per cent of all severely malnourished children admitted to our nutrition centre have HIV/AIDS. About 60 per cent of these are co-infected with tuberculosis. Over 75 per cent of all deaths in the nutrition centre occur in children with HIV infection.
Would you know what the case fatality for severe malnutrition is in hospital wards in Uganda?
As I mentioned, case fatality rate in our hospital is between 10-20 per cent. There are not many such centres in the country, but studies by colleagues reported a case fatality rate of 24 per cent at Mulago National Referral Hospital (2). Similarly, Babirekere and colleagues report case fatality rates of 18 per cent in oedematous malnutrition and 22 per cent in severely wasted children (3) among severely malnourished Ugandan children admitted in a hospital. Many children with malnutrition are still dying in hospital wards in Uganda.
Would you say health professionals especially those who care for sick children know and follow guidelines on malnutrition management such as those from WHO?
There is a lot of effort in trying to follow WHO and nationally adapted guidelines in hospitals to care for very sick children with severe malnutrition. But only about three centres in the country have specific nutrition wards and the resources are very limited. Following protocols adequately is difficult even when the knowledge, skills and will are present. Most other hospitals have no specialised nutrition services and little is specifically done in accordance with guidelines. The Ministry of Health is continually providing guidance in terms of policies, guidelines and supervisory support and has recently developed an integrated management of acute malnutrition – the IMAM protocol.
How informed are health professionals regarding current issues in addressing malnutrition in children such as the Johannesburg resolution and he ANEC 4 Nairobi declaration?
Current updates addressing malnutrition are lacking among most health professionals except those in university teaching hospitals and those with specific interest in nutrition or those involved in the few nutrition centres.
Would you agree that doctors and other health professionals should know how to identify, treat and prevent malnutrition among children?
I strongly agree. Malnutrition is such an important component of the disease burden in Uganda. Every health worker involved in the care of children at every level should have adequate knowledge and skills to identify, treat and prevent malnutrition in children.
Renewed national interest
What are the current practices regarding treating and preventing malnutrition among children in Uganda?
There is renewed national interest in the management of malnutrition, at Ministry of Health level. Teams are being established in all departments of hospitals that interact with children to identify, appropriately refer or manage children with malnutrition. The necessary logistical and infrastructural support is still largely lacking. Otherwise most facilities refer severely malnourished children to regional referral hospitals for specialised care.
Prevention efforts are lagging far behind, with policies and guidelines not being translated sufficiently into action. As a result, socio-cultural practices and beliefs, poverty and ignorance, adverse weather and regional differences still curtail any efforts at preventing malnutrition in children.
Scaling up: training is crucial
How can we scale up the treatment and prevention of malnutrition in Uganda and sub Saharan Africa as a whole?
Community based therapeutic centres, with regional hospital based referral facilities, may be the way to scale up treatment and prevention of malnutrition. Community based therapeutic centres are essentially accessible outreach centres with the capacity to assess and refer severe or complicated malnutrition, or to treat moderate or uncomplicated malnutrition. They also provide follow-up opportunities for those recovering from severe malnutrition. These centres can also train community leaders to identify children at risk of malnutrition, or with moderate to severe malnutrition, for appropriate management. They are accessible to communities and mothers.
Hospital based therapeutic centres provide referral, technical, supervisory, research and capacity development services. The national government should give a higher priority to malnutrition and should scale up funding and logistical support to the community and hospital-based centres described above.
The way forward
In your opinion what should be the way forward in addressing malnutrition in Uganda in order to achieve the Millennium Development Goals?
The community based and facility based therapeutic centre approach is one way. It is within Uganda's means to implement since there is an already established health care system. However, it is now too late to achieve the MDGs in this area. Food security and a gradual transformation of the population's knowledge and incomes will improve the care of children. Weaning practices need to be harmonised across the regions of Uganda, with breastfeeding promotion upheld.
The gains from Uganda's fight against HIV need to be consolidated.Mother to child transmission of HIV must be reduced by adopting and implementing the new WHO guidelines, if we are going to cut down the contribution of HIV to childhood malnutrition. Child spacing and a reduction in Uganda's fertility rates by increasing availability and uptake of family planning methods to the rural communities is another way.
Thank you
My conclusion
Elias raises key issues. Many of these have been with us for far too long. Malnutrition is still a major problem in Africa, and HIV/AIDS is contributing to this. Many children still die from malnutrition and HIV related complications. The achievements of Elias, Flo and others are bright lights of hope, but such work needs scaling up. If you would like to know more and want to be involved with addressing malnutrition, please visit the international malnutrition task force, where I work currently based in Southampton in the UK, at www.imtf.org.
Most of the malnourished children also have HIV infection. This needs to be addressed as well. What is happening to these children in this regard? What are the guidelines for anti-retroviral treatment? Are anti-retroviral drugs available and in what sense are they universally accessible? Are there efforts to ensure real universal accessibility and to back the many promises with action? I will explore these and other issues next month. Stay with me on this journey.
References
- Uganda Bureau of Statistics (UBOS) and Macro International Inc. 2007. Uganda Demographic and Health Survey. 2006. Calverton, Maryland, USA: UBOS and Macro International Inc.
- Bachou H, Tylleskar T, Downing R, Tumwine JK. Severe malnutrition with and without HIV-1 infection in hospitalised children in Kampala, Uganda: differences in clinical features, haematological findings and CD4+ cell counts. Nutrition Journal 2006; 5, 27.
- Babirekere-IrisoE, Musoke P &Kekitiinwa A. Bacteraemia in severely malnourished children in an HIV-endemic setting. Annals of Tropical Paediatrics 2006; 26 (4):319-28.
Acknowledgement and request
You are invited please to respond, comment, disagree, as you wish. Please use the response facility below. You are free to make use of the material in this column, provided you acknowledge the Association, and me please, and cite the Association’s website.
Please cite as: Annan R. African food taboos, and other items. [Column]. Website of the World Public Health Nutrition Association, April 2011. Obtainable at www.wphna.org
The opinions expressed in all contributions to the website of the World Public Health Nutrition Association (the Association) including its journal World Nutrition, are those of their authors. They should not be taken to be the view or policy of the Association, or of any of its affiliated or associated bodies, unless this is explicitly stated.
This column is reviewed by Geoffrey Cannon.
I would like to express my gratitude to Dr Elias Kumbakumba for granting this interview. We appreciate your work addressing malnutrition in Uganda and we hope that others will join the train. There much to learn from the experiences you have shared with readers all over the world.