2012 March blog
Reggie Annan

Ghana. This month I continue with my coverage of the zero tolerance for maternal deaths during childbirth campaign in Africa, initiated by Ghana's first lady Naadu Mills. I look at the trends, direct and underlying causes, and lessons we can learn from countries that have succeeded in reducing these unnecessary deaths. Is zero tolerance possible and how can it be achieved? Once again enjoy this intriguing sight above from beautiful Africa.
Deaths during childbirth
How to end this scandal
I decided to write about maternal mortality last month, because in my short time back home in Ghana I personally have heard of a couple of women; well to do, educated, enlightened, and probably without any major complications during pregnancy, who died during childbirth. Since then a similar case has been brought to my notice. I thought to myself that Ghana has a crisis situation that probably has not been seen as such yet. In fact it is a crisis right across Africa.
Globally one woman dies from complications in childbirth every minute making about 529,000 each year, the vast majority of them in lower-income countries. For every woman who dies, approximately 30 more suffer injuries, infection and disabilities in pregnancy or childbirth (1). For instance there are birth-related disabilities that affect many more women and go untreated, like injuries to pelvic muscles, organs or the spinal cord. At least 15 million women a year are reported to incur this type of damage. The cumulative total of those affected has been estimated at 300 million, or more than a quarter of adult women in the South (1).
In 2000, compared with high-income countries where a woman had a mere 1 in 4000 risk of dying during childbirth, in sub-Saharan Africa the figure was 1 in 16 (1). Hence Millennium Development Goals 4 and 5, which were endorsed in 2001 by 147 heads of states, to reduce child mortality rate by two-thirds, and maternal mortality ratio by three-quarters, between 1990 and 2015. But the figures have not changed much since then. If anything the situation is getting worse.
Hear this: 'The expert advice is clear: maternal mortality in Africa is a crisis and it is a crisis which is likely to worsen. Africa has the highest maternal mortality rate in the world. Experts on reproductive health have painted a grim picture of maternal and child health in the region and warned that the situation could worsen in the next decade if no immediate remedial actions are taken by Africa's governments and development partners' (2).
Let's look at the causes of maternal mortality. They have not really changed over many years. Also, how was maternal mortality dealt with in the North, and what can Africa learn ? First, the causes.
Immediate and underlying causes
No change in 20 years
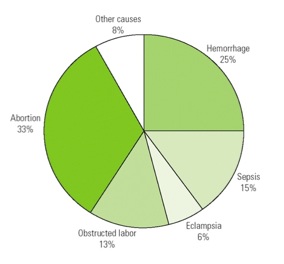
As shown from the chart above, by 1992, the immediate causes of maternal mortality in lower-income counties in order of incidence were, in percentages, unsafe abortions (33), haemorrhage (25), sepsis (15), obstructed labour (13), eclampsia (6) and others (8) (3). A more recent report positions the leading cause of death and disability among women of reproductive age in lower-income countries as complications of pregnancy and childbirth (1). The complications listed here are haemorrhage, infection, obstructed labour, hypertensive disorders in pregnancy, and complications of unsafe abortion. In Africa and other countries where malaria is endemic, anaemia increases the risk for maternal and infant mortality and developmental problems for babies. In Sub-Saharan Africa, HIV infection is an increasing threat to mother-to-child transmission of HIV, and also is a major cause of maternal mortality. The direct causes of maternal deaths have not changed much in 20 years
Underlying causes
There are also underlying causes, which can be termed, causes of these causes. Probably the main reason why direct causes have persisted is because efforts have not been focused on the underlying causes.
Insufficient care during pregnancy and delivery is a major underlying factor. This exists prior to pregnancy and will affect the pregnancy process and its outcome. There are also long term problems that make girls in some African countries prone to problems as women (4). These are to do with attitudes, mind-set and even how the society is run.
The underlying causes include general health care and delivery, the nutrition and health of women, political and governance issues, and the socio-economic status of women in particular.
Poor health care access and delivery

Sufficient care during pregnancy means that women seek antenatal services from qualified and trained personnel, to ensure that they are healthy throughout the pregnancy. Adequate access to skilled care during pregnancy, childbirth and the first month after delivery is essential to ensuring good care and saving lives.
Lack of health delivery close enough to communities is a reason why women seek care from untrained personnel. About half of all deliveries in the developing world are attended by unskilled birth attendants. In Africa only just over two-fifths of births are attended by skilled personnel (5). This means that for almost three-fifths of women giving birth, there are no skilled personnel or equipment to deal with complications such as bleeding during delivery. It is more likely that those with access to skilled personnel live urban areas, more likely to be educated, enlightened and well to do: women who know and can afford to take good care of themselves when pregnant. Therefore they are less likely to have problems or problems are identified and dealt with in a timely manner.
Many women living in remote areas like the one pictured above walk several kilometres to access health care. Will they do that if pregnant or in labour? In Ghana, women in the Upper Manya District were reported to be attending prayer camps and healing centres for antenatal care, instead of health centres or clinics. The reason was because they have to trek long distances before getting access to a medical facility (6).
Poor governance
African governments have usually had inadequate public health budgets. The percentage of GDP (gross domestic product) devoted to health in sub-Saharan Africa remains at between 1 and 3.7 per cent (5). This is not just because many African countries are impoverished, with inadequate public funds. Two other reasons are wrong priorities, and politicians' quest for power. For instance, money spent on arms is more than money spent on health. African leaders who want to remain or win power often do not mind going to war and allowing the destruction and collapse of the welfare and health systems and structures which have been built over many years. This is unconscionable.
Low status of women
Poor socio-economic status of women had contributed to their general low status. For women who live on less than the equivalent of $US 2 dollars a day in a remote village in Somalia, travelling long distances is not only costly but means that livelihood is lost. A woman may also need to leave her other children at home who equally require care to travel for antenatal services. So she is too poor and too discouraged.
Unsafe abortions are also high among adolescents in Africa and low status contributes. For instance, poverty and ignorance can both lead to unwanted pregnancies, the desire to abort and the practice of unsafe abortions. In certain African societies decisions for family planning and birth spacing may not be made by a woman. She cannot choose family planning by herself so if her fertility is high, the number of times she gets pregnant, how close one pregnancy is to the other, and how well she is to carry the pregnancy are not decisions she can make. Also sometimes she may want to have more children in order to compete with her rivals.
A witness from Somalia has said: 'Once the girl is married, immediate and frequent fertility is expected of her, without taking into consideration whether or not her body can take care of the baby she will conceive. Our women, therefore, produce as many children as they can, to ensure their place in their new home. In my work, I often witness women having baby number 9 or 10, and also some having baby number 12, 13, 14, 15 or 16 and, once, baby number 21' (4)
Poor education

How many of these girls pictured above are being guided to guard against problems during womanhood? Education is important to health. The higher the level of education, the more likely a woman is to make good decisions. But when parents have to decide which of their children can be sent to school, because funds are limited in the family, it is often the girls who are left behind. This is more common in rural villages but in the urban areas my observation is that parents are also more eager to educate their male children especially when they reach secondary and tertiary levels.
Conversely, the lower their education level of a girl or woman, the higher her risk of health problems, including those associated with reproductive life. An illiterate woman is not able to seek her rights for health care because she may not even be aware that she has any rights at all. Some do not know the benefits and risks of certain behaviours. If she lives in the village, it is also more likely for other women to advise a pregnant woman not to seek health service, saying it is not necessary, I had my children without going to the hospital.
Poor nutrition
Poor nutrition among women is a problem that starts right from childhood. There is increasing degradation of the environment in sub Saharan Africa, and there are too many war torn zones in Africa. These mean displacement of people from their source of livelihood, and also unnecessary expenditure on arms. Girls in poorer settings within such regions are almost bound to have poor nutritional status. They are likely to grow into womanhood stunted, prone to obesity, anaemic and with a narrow pelvis.
Even in African societies where there is relative peace, a boy child may still be preferred. This makes the girl child vulnerable and unprepared for successful childbirth. Knowledge of the developmental origins of health and disease tells us that during pregnancy the foetus is programmed nutritionally. If a woman who is poorly prepared because of her past exposures as a girl, also has poor nutrition during pregnancy due to poverty or ignorance the outcome could be a calamity.
UNICEF's approach in Africa
How best to prevent maternal deaths

Here is what UNICEF, the world body mandated to work with issues of the health and welfare of women and children, is doing. Four types of intervention are used. These are helping improve emergency obstetric care; laying the foundations for good prenatal care; helping preventing mother-to-child HIV; and getting girls to school (1). The photo above shows an aspect of prenatal care. The most important policies and actions for safe motherhood are to make sure that a trained provider with midwifery skills is present at every birth; that transport is available to referral services; and that quality emergency obstetric care is available.
Lack of good prenatal care often results in untreated hypertensive disorders leading to death and disability, or unmarked malnutrition, including untreated iron deficiency anaemia which is associated with some 111,000 maternal deaths each year. Providing women with information on signs of pregnancy complications, on birth spacing, timing and limiting for nutrition and health, and on improving the nutritional status of pregnant women, are goof foundations. Programmes that promote and help provide anti-malarial therapy and insecticide-treated bed nets, tetanus immunisations for pregnant women, micronutrients to stave off anaemia and birth defects are also good approaches.
All governments should provide adequate universal primary school education. Educating girls for six years or more greatly improves their prenatal care, postnatal care, and childbirth survival rates. Educated girls have higher self-esteem, are more likely to avoid HIV infection, violence and exploitation, and spread good health and sanitation practices to their families and throughout their communities. An educated mother is more likely to send her children to school.
Policies in the North
Lessons from recent history

Maternal deaths have not always been been low in higher-income countries. We in Africa can learn from what has been achieved elsewhere. I have been researching, and have found an important presentation made in 1988 at a maternal mortality meeting held in the US (7).
High maternal mortality was common in the North until the mid-1930s. From around 1937 rates began to decline, and within 20 years there were no inter-country disparities. Current rates are now between one-fortieth and one-fiftieth of what prevailed prior to 1930. The single most important determinant of this reduction was the overall standard of maternal care provided by birth attendants, with poverty and malnutrition playing a part.
What Europe and the US did
Fever was a common cause of maternal deaths in Europe and the US before the mid 1930s, accounting for over 40 per cent of deaths. When asepsis practices were introduced in hospitals in Europe, it greatly reduced these deaths.
Between the 1920s and 1940s births were supervised by trained midwives in home deliveries and deaths were reduced drastically. Thus in the US, midwives in the Kentucky Frontier Nursing Service travelled on horseback to assist with deliveries which were all at home in a poor farming community with low living standards. Pictured above is a midwife sitting sidesaddle on a horse at Blackall, Queensland in the US.
In the UK, rural nurses from the Queen's Institute of Nursing, an organisation with highly trained and supervised midwives were involved in record-keeping and home deliveries (7).
Contrary to what you may be thinking, maternal mortality was not associated with social class. In fact an unexpected inverse relationship was found in the UK It was thought that unnecessary interference with the delivery process was the reason; those in upper social classes were more likely to be delivered by physicians with sophisticated equipments. Malnutrition was only a weak determinant of maternal mortality in this period. It was care during parturition that mattered most.
What Africa needs to do
Judging from history, what really worked was not sophisticated birthing equipment, the presence of physicians, or even social class generally. Maternal mortality was reduced by providing trained and skilled birth attendants who provided a high standard of care during delivery, while preventing and treating fever. For me this evidence shows why the high maternal mortality in both villages and urban areas in Africa is so high. We need every delivery to be attended by midwives, or by trained and skilled nurses with midwifery skills.
Africa now is where the US and Europe were in the 1930s. I therefore believe that what they did to prevent maternal deaths is what we should do. At the same time, other underlying factors must not be neglected.
If there is one major intervention we can implement in Africa, it is to ensure that all births are attended to by midwives or trained nurses with midwifery skills, in an infection-free environment, with adequate standards of care. From 1990 to 2000, the percentage of births attended by a medical professional in Asia rose by 35 per cent. In Sub-Saharan Africa, it only improved by 5 per cent (1). It is not surprising that maternal mortality is highest in our region. But yes, zero tolerance to maternal deaths is possible and is achievable?
References
- UNICEF Millennium Development Goals. Obtainable at http://www.unicef.org/mdg/maternal.html.
- Grieco M, Turner J (2005). Maternal mortality: Africa's burden. Toolkit on Gender, transport and maternal mortality. Vs4-04-2005. Accessed at http://www4.worldbank.org/afr/ssat[/Resources/HTML/Gender-RG/.
- WHO (1992). Major Causes of Maternal Mortality in Sub-Saharan Africa.
- Ismail E (2008) On Maternal Mortality, Why Africa Falls So Far Behind. Obtainable at http://www.rhrealitycheck.org/blog/2008/10/02/on-maternal-mortality-why-africa-falls-so-far-behind.
- Dzadeyson E (2007). Study on maternal mortality and neonatal morbidity in Africa. Rural Integrated Relief Service-Ghana. Obtainable at http://www.who.int/pmnch/topics/health_systems/rirs_ghana/en/index.html.
- Peace FM Online. December 2011. Pregnant women attend prayer camps for ante-natal care. Accessed at http://news.peacefmonline.com/health/201112/86196.php.
- Loudon I. Maternal mortality in the past and its relevance to developing countries today. American J of Clin Nutr 2000;72(1): 241s -246s.
Acknowledgement and request
You are invited please to respond, comment, disagree, as you wish. Please use the response facility below. You are free to make use of the material in this column, provided you acknowledge the Association, and me please, and cite the Association’s website.
Please cite as: Annan R [Column]. Deaths during childbirth. How to end this scandal. Website of the World Public Health Nutrition Association, March 2012. Obtainable at www.wphna.org.
The opinions expressed in all contributions to the website of the World Public Health Nutrition Association (the Association) including its journal World Nutrition, are those of their authors. They should not be taken to be the view or policy of the Association, or of any of its affiliated or associated bodies, unless this is explicitly stated.
This column is reviewed by Geoffrey Cannon.